Fractures
Stress fractures are very small, fine breaks in a bone. They most often occur in the bones of the lower legs and feet. Stress fractures are caused by repeated shock to the bone. They are most common with high-impact sports, such as basketball, tennis, and running. Poorly cushioned shoes, hard surfaces, and a sudden increase in exercise time or intensity can contribute.
Your doctor will ask you questions about your activities and your health history. Be sure to tell your doctor about any changes to your exercise or training routine, such as a change in playing surface. Stress fractures don’t always show up on X-rays, so your doctor may order bone scans, and/or magnetic resonance imaging (MRI).
Rest is the best way to treat a stress fracture. If the leg or foot is not rested, the fracture will likely become worse and harder to heal. To ensure proper healing:
- Replace high-impact activities with low impact ones, such as swimming or cycling, until the fracture has healed. This takes about six to eight weeks.
- Use ice, heat, and over-the-counter pain relievers as directed by your doctor.
- Use crutches as directed by your doctor if walking is painful.
- Wear a special walking cast or shoe if your doctor recommends. These can improve healing of certain types of fractures.
- Ease back into activity when your doctor gives you the okay.
To help prevent stress fractures:
- Ease into new sports activity. If you run, don’t start at five miles a day. Instead, start with one mile and gradually increase your miles.
- Alternate your activities. Work low-impact activities into your routine.
- If you’re a woman, be sure to get enough calcium and vitamin D. Ask your doctor about supplements.
- Be sure your shoes are right for the activity you’re doing. Don’t wear shoes that are worn out.
- Stop an activity if you have pain or swelling. Rest until the pain goes away.
Ruptured Tendon
The largest and strongest tendon in the body, the Achilles tendon connects the two main calf muscles to the heel bone. Common injuries include tendonitis (inflammation), tendinosis (degeneration) and rupture. Tendonitis and rupture can occur from overuse of the tendon during work or athletic activities or an injury to the lower leg or ankle. Tendinosis is chronic and degenerative; continuous stress creates micro-tears and a breakdown of collagen tissue within the tendon. The main function of the Achilles tendon is the transmission of power from the calf muscles to the heel and the foot. This makes it possible to flex the foot (plantar flexion). This movement is crucial for toe off of the foot when walking and running. The Achilles tendon is also involved in supination (twisting onto the outer edge) of the foot. The Achilles tendon must withstand very high forces, especially when jumping and landing. For example, a force equal to eight times your own body weight acts on the Achilles tendon when running.
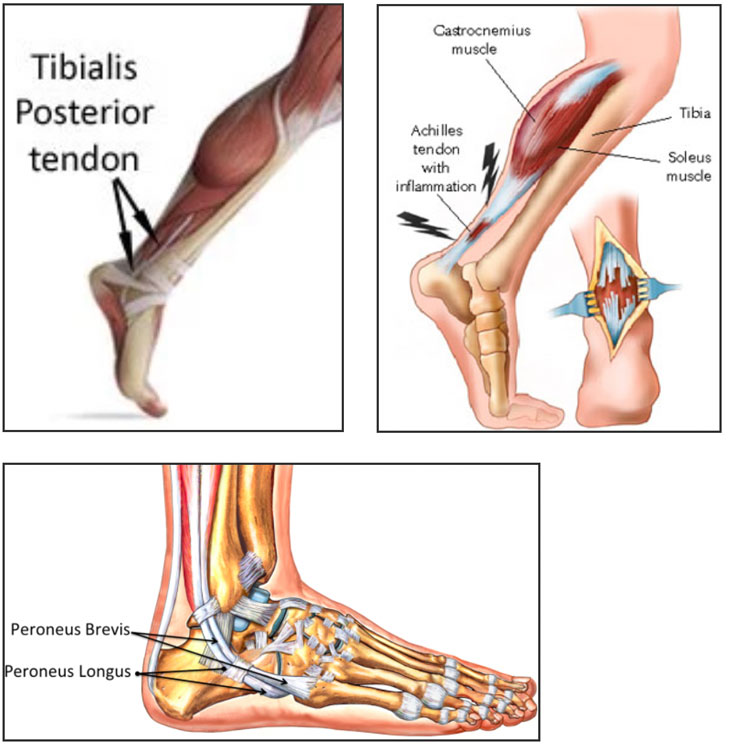
The posterior tibial tendon is one of the most important tendons of the leg. A tendon attaches muscles to bones, and the posterior tibial tendon attaches the calf muscle to the bones on the inside of the foot. The main function of the tendon is to hold up the arch and support the foot when walking.
The two peroneal tendons in the foot run side by side behind the outer ankle bone. One peroneal tendon attaches to the outer part of the midfoot, while the other tendon runs under the foot and attaches near the inside of the arch. The main function of the peroneal tendons is to stabilize the foot and ankle and protect them from sprains.
While tendonosis and tendonitis are usually treated conservatively with injections, physical therapy, NSAIDS (non-steroidal anti-inflammatories) and immobilization, ruptures often require surgical repair. Surgical intervention can be accomplished via direct repair or various tendon transfers. New surgical techniques allow patients to return to pre-injury activity much quicker than in the past. Current techniques include smaller incisions and stronger repair, which allow for shorter recovery time and much better outcomes.
The Achilles, posterior tibial and peroneal tendons are the most commonly ruptured tendons in the foot and ankle. Other less commonly ruptured tendons include tibialis anterior, flexor digitorum (longus and brevis), flexor hallucis (longus and brevis), extensor digitorum (longus and brevis) and extensor hallucis (longus and brevis).
Dislocation
A dislocation is an injury to a joint in which the ends of your bones are forced from their normal positions. Dislocations can be complete or partial-such as an ankle sprain. This painful injury temporarily deforms and stiffens your joint.
Dislocation in the foot and ankle most commonly occurs in toes. Other sites include ankle, midfoot (Lisfranc), and the subtalar joints. If you suspect a dislocation, seek prompt medical attention to return your bones to their proper positions. When treated properly, most dislocations return to normal function after several weeks of rest and rehabilitation. However, some joints, such as your ankle, may have an increased risk of repeat dislocation
A dislocated joint can be swollen, bruised or discolored, visibly deformed or out of place, intensely painful and stiff or immovable. Since the symptoms of a dislocated joint mimic a broken bone, it can be difficult to tell a broken bone from a dislocated bone. For either type of injury, get medical help right away. If possible, ice the joint and keep it immobile while you’re waiting to be seen. Dislocations can occur in contact sports, such as football and hockey, and in sports in which falls are common, such as downhill skiing, gymnastics and volleyball. Basketball players and football players also commonly dislocate joints in their foot and ankle by accidentally striking the ball, the ground or another player. A hard blow to a joint during a motor vehicle accident and landing on an outstretched leg and foot during a fall are other common causes.
Diagnosis and Treatment:
Besides examining your injury, your doctor might order the following: xray, MRI or CT scan. An X-ray of your joint is used to confirm the dislocation and may reveal broken bones or other damage to your joint. A CT-Scan or MRI can help your doctor assess damage to the soft tissue structures around a dislocated joint.
Treatment of the dislocation depends on the site and severity of your injury. It might involve: Reduction. Your doctor might try gentle maneuvers to help your bones back into position. Depending on the amount of pain and swelling, you might need a local anesthetic or even a general anesthetic before manipulation of your bones. Immobilization. After your bones are back in position, your doctor might immobilize your joint with a splint or sling for several weeks. How long you wear the splint or sling depends on the joint involved and the extent of damage to nerves, blood vessels and supporting tissues. Surgery. You might need surgery if your doctor can’t move your dislocated bones into their correct positions or if the nearby blood vessels, nerves or ligaments have been damaged. Surgery may also be necessary if you have had recurring dislocations, especially of your ankle. Rehabilitation. After your splint or sling is removed, you’ll begin a gradual rehabilitation program designed to restore your joint’s range of motion and strength.
Puncture Wound
A puncture wound of the foot is where there is a small entry hole caused by a pointed object, such as a nail, insulin needle toothpicks or piece of glass that you’ve stepped on. It is very important to get proper treatment within the first 24 hours due to the high rate of infection. Even if you have gone to an emergency room for immediate treatment of your puncture wound, see a foot and ankle surgeon for a thorough cleaning and careful follow-up. The sooner you do this, the better.Infection is the most common complication of puncture wounds. Sometimes a minor skin infection can develop into a bone or joint infection. A minor skin infection may develop in two to five days after injury. The signs of a minor infection may include soreness, redness, and possibly drainage, swelling, and warmth. You may also develop a fever. If these signs have not improved, or if they reappear in 10 to 14 days, a serious infection in the joint or bone may have developed. You will then have to been seen on an emergency basis by either your foot surgeon or the local emergency room.
Foreign Body
A foreign body (FB) is any substance that is not naturally part of the body. For example, a patient who is walking without shoes and experiences a sharp, sudden pain in the foot may have a needle, toothpick, or any other similar type of FB. X-Rays taken of the foot may or may not show the FB. MRI or ultrasound may be needed in those cases. It is very important to see your foot doctor or go to the emergency room to get treatment to avoid getting a serious infection.
